Osteoporosis and spine health
Osteoporosisis a disease that decreases bone quality. It is a silent condition that often goes unrecognized unless it leads to fractures. Due to this risk, appropriate screening is needed. If a fracture has occurred, it may require surgical treatment. Some osteoporotic fractures, first of all hip fractures, have been shown to increase the risk of dying.
Symptoms of osteoporosis
Fracture of the spine bones (vertebral compression fractures) is the most common manifestation of osteoporosis, followed by hip and wrist fractures.
Fractures of the long bones, like hip and wrist, are usually easily diagnosed: there is trauma followed by pain, deformity and inability to use the arm or leg. With spine fractures, commonly there is back pain, which may start after very minimal trauma, like stepping off a curb or sneezing. Sometimes, there is no apparent injury at all.

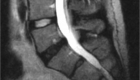
Figure 1 Osteoporotic vertebral fracture at L1 (red arrow); normal shape of spine bones, vertebrae (yellow arrows)
Multiple vertebral fractures with time may lead to loss of height and development of a back hump and difficulties standing straight.

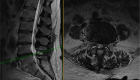
Figure 2 Progressive spine deformity as a result of multiple osteoporotic vertebral fractures
Osteoporosis may develop over the years without fractures and cause no symptoms. Hence, it is very important to screen for it.
Diagnosing osteoporosis
Bone density scan, also called DEXA, is the main diagnostic tool used to diagnose osteoporosis. DEXA produces a number based on the bone quality, called the T-score. T-score of zero is equivalent to bone quality of a young adult in her twenties. Negative number of T-score indicates deterioration of the bone quality. T-score between -1.5 and -2.5 indicates osteopenia. T-score of -2.5 and below indicates osteoporosis
It is also possible to estimate the risk of having osteoporosis and resulting fractures using questionnaires. Here is a link to the most widely used online tool, FRAX: https://www.sheffield.ac.uk/FRAX/tool.aspx?country=9
Who is at risk for developing osteoporosis?
There are several factors that increase the risk of developing osteoporosis:
- Age over 65 years
- Female sex
- Low body mass
- History of previous fractures in the patient or parents
- Smoking and alcohol consumption
- Rheumatoid arthritis
- Use of steroids
Who should be tested for osteoporosis?
Current recommendations are based on age. Women 65 years of age or older and men 70 years of age or older should be tested for osteoporosis. If there are additional risk factors, the age is lowered to 50 for both men and women.
Treatment of osteoporosis
There are several medications that treat osteoporosis once it is diagnosed. They have different mechanism of action but broadly speaking one group prevents bone loss and the other helps new bone to form.
Some of the most widely know medications from the “prevention” group are bisphosphonates, for example, Alendronate (Fosamax) and Zoledronic acid (Reclast). A new medication with a different mechanism of action is called Denosumab (Prolia).
In the “grow new bone” group there are currently only two medications, Forteo and Tymlos. Both of them are injected once a day using a portable pen, similar to epipen or insulin pen.
Prevention of osteoporosis
Bone mass peaks in the early 20’s and then gradually declines throughout life. As such, there are two strategies we can use to decrease chances of osteoporosis later in life:
- Maximize amount of bone in the childhood and teen years by healthy diet and staying physically active and;
- Slow down bone loss after the bone mass peaks.
We recommend you to stay physically active and take moderate doses of calcium and Vitamin D, have enough (but not too much) exposure to sun. High doses of calcium may lead to kidney stones.
What other conditions may cause weak bones?
Along with osteoporosis, bones may weakened by other processes that need to be ruled out prior to beginning any treatments. Bone cysts, tumors and infections may all weaken the bone.Quote
How does osteoporosis affect my plans of having spine surgery?
In cases when spine fusion with instrumentation is planned, weak bones may lead to the screws pulling out and failure of fixation. For this reason we routinely screen patients, who have plans for spine surgery and when needed treat osteoporosis for at least three months before operation.
What are the treatments of osteoporotic vertebral fractures? Do I need to have surgery?
Unlike hip fractures, in which surgery is almost always needed, vertebral fractures heal on their own in most cases.
If the symptoms persist after a month or so, there is an option to reinforce the fractured bone by injecting bone cement. This is called vertebral augmentation. There are two types of surgical vertebral augmentation: vertebroplasty and kyphoplasty.
I take calcium and Vitamin D supplements and drink a lot of milk. Am I protected against osteoporosis?
This has been a long belief that Calcium and Vitamin D supplementation is important for prevention of osteoporosis. Recent large studies show no significant benefit.
Large doses of calcium may lead to kidney stones, however. This means that you should still take supplementation but be cautious about the dose.
Can men develop osteoporosis?
Yes. Even though we are used to hearing about osteoporosis in menopausal women, men may be affected too. Low testosterone levels may increase the risk.
Is there a difference between osteoporosis and osteoarthritis?
This question arises from some confusion because of similarity of the two terms.
Osteoporosis is poor bone quality that may lead to fractures or failure of orthopedic implants.
Osteoarthritis (or just arthritis) is inflammation of joints, like hip or knee. This word is often used to indicate arthrosis, a condition when joints deteriorate because of wear and tear. Arthritis of spine is called spondylosis.
If you have additional questions about spine health, contact us or request an appointment by filling out an online form. Stop letting spine pain control your life. Schedule your consultation with me today and take the first step towards lasting relief. Your journey to a pain-free life begins now. Click here to book your appointment.